A catheter often seen on the arm of oncology patients is the PICC, which offers advantages such as safety, convenience, minimal incision, and low infection rates. For many patients, a safe and effective venous access is their lifeline.
Recently, our medical team once again successfully performed the peripherally inserted central catheter (PICC) insertion procedure, solving the crucial challenge of venous access for a breast cancer patient undergoing chemotherapy.
Cen, a breast cancer patient, has been battling the disease for nearly four years. Due to the long-term need for pain management with a PCA pump, she required a central venous access. Previously, she had a port-a-cath inserted and removed, and two PICC lines inserted, with one of them expiring after a year. Despite this, Cen chose to come to our hospital for the reinsertion of the PICC line.
Under the leadership of Nurse Zhang Hong, the nurse team carefully assessed Cen's situation using ultrasound. It was determined that the PICC line in her right arm needed to be preserved for pain management with the PCA pump. However, the veins in her left arm were unsuitable for catheter insertion due to their small size, and there was a scar from a previous port-a-cath placement below the left clavicle. Nurse Zhang Hong concluded that inserting the catheter would pose certain difficulties, including challenges with puncture and advancement of the catheter. She communicated this to Cen, who reassured her by saying, "I understand. Please continue. I trust you."
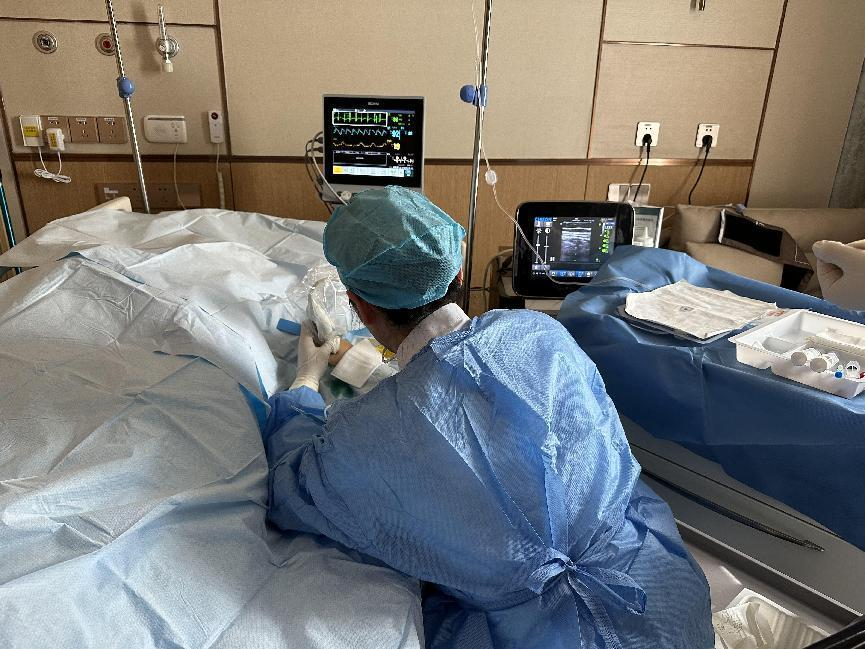

Nurse Zhang Hong performed the PICC insertion procedure for Cen. Opting for a cephalic vein puncture, she skillfully advanced the guidewire, introducer needle, and catheter to the predicted length. However, during electrocardiogram-guided positioning, there was an absence of the expected high, sharp P-wave preceding the QRS complex. Drawing upon her years of experience, Nurse Zhang Hong suspected catheter misplacement. Ultrasound assessment of the left internal jugular vein revealed no presence of the catheter, which typically poses the highest risk for catheter misplacement. The nurse team then accompanied Cen to the radiology department for imaging and catheter adjustment, discovering that the PICC line had looped around the mid-clavicular region before extending to the axilla.
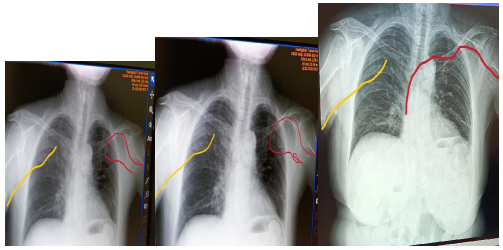

Nurse Zhang Hong, along with Nurses Li Xiaofeng and Tang Xiaojun, under Nurse Zhang's guidance, employed various techniques to adjust the catheter. With Cen's cooperation, their efforts paid off, and the catheter tip was successfully positioned at the optimal T7 level. Cen's PCA pump was relocated from her right arm to the newly inserted left PICC line, and the PICC line on her right side was removed.
"Cen was very cooperative throughout the catheter adjustment process, without a single complaint. It's because of this trust that we were able to succeed," recounted Nurse Li Xiaofeng, remembering clearly the scene on the day Cen was admitted in October 2021. Despite having previously spoken with Cen's family over the phone to understand her condition and the purpose of her hospitalization, Nurse Li was still shocked and distressed to see Cen in person. At 160cm tall, she weighed only 40kg, unable to sit or stand due to pain, and relied on a makeshift stretcher made by her family. She seemed fragile, as if a gust of wind could blow her away. Upon admission, it was discovered that Cen was covered in fentanyl patches for pain relief, along with five other pain medications, yet her pain remained at an 8 out of 10, leading to issues such as constipation, poor sleep, and malnutrition.
After admission, the medical team at Guangzhou Royal Lee Cancer Center collaborated with Cen and her family to devise a treatment plan. Priority was given to addressing her pain through intravenous PCA pain management, nutritional support, and alleviating constipation, while closely monitoring for adverse drug reactions. However, the immediate challenge was her venous access. Previously, she had a port-a-cath inserted elsewhere, which was subsequently removed. Hence, the decision was made to insert the first PICC line for Cen to initiate intravenous pain management promptly. With pain relief from the intravenous PCA, Cen's sleep, diet, and constipation improved. Once her pain was alleviated, discussions with her family and Cen led to planning for continuous PCA pain management, understanding that she couldn't stay in the hospital indefinitely. The hospital leadership prioritized this issue, implementing a protocol where Cen could be discharged with the PCA pump while the hospital remotely monitored its usage to ensure safe medication administration. Additionally, arrangements were made for local community healthcare services to provide routine catheter care, with community nurses visiting Cen at home.
After a period of pain management and treatment for the primary disease, Cen's frail body, which initially weighed 40kg, increased to 58kg, enabling her to walk freely and manage her daily activities independently. Cen's quality of life had significantly improved.
Over the course of more than two years, the medical team at the hospital reinserted the second and third PICC lines for Cen. The mutual trust and care between the patient and the medical staff were profoundly touching, a testament to empathy.
"They have given me hope for life, allowing me to return to my family and enjoy the happiness of family life," Cen said emotionally.
